Just 0.3 per cent of Covid-19 cases in Singapore admitted to ICU


While Covid-19 cases in Singapore have surged past 50,000, only a tiny fraction of those who fell ill - just 128, or 0.3 per cent - have been admitted to the intensive care unit (ICU) as of Monday.
Experts said years of investment in healthcare, as well as a well thought out and executed strategy to keep infection numbers low, have helped to ensure the Republic has one of the world's lowest ICU admission - and fatality - rates from Covid-19.
In the last two weeks, there has been no admission to the ICUs, with the last patient discharged on July 14.
Of those who were in the ICU, more than three quarters, or 98, have fully recovered and been discharged.
Another eight are recovering in general wards in the hospital.
Still, not everyone got well, with 18 patients dying from Covid-19-related reasons while four died of other causes.
Until now, Singapore has had 27 Covid-19-related deaths.
This makes for a case fatality rate of less than 0.1 per cent - an extremely low percentage compared with that of other developed nations.
According to John Hopkins University on Wednesday, the United Kingdom ranked highest in case fatality rate - an indication of how likely a Covid-19 patient will die in the country - at 15.2 per cent.
Mexico ranked second at 11.1 per cent and Iran came in third at 5.5 per cent.
An extremely low case fatality rate like in Singapore is a reflection of the nation's high quality of healthcare, suggesting that doctors and ICU specialists are well-trained and prepared to treat critically ill patients so they have a better chance of survival, said Dr Phua Kai Hong, an adjunct senior research fellow with the Institute of Policy Studies at the Lee Kuan Yew School of Public Policy.
[[nid:497049]]
It also reflects how well-stocked and equipped ICUs are so patients are able to receive timely and proper utilisation when needed, Dr Phua added.
"As Covid-19 slowly subsides, and if the quality of care is maintained, the case fatality rate in Singapore would look better and better when compared with other countries," he said, while noting there will be some adjustments in tallying deaths when the pandemic finally subsides.
The low death rate and ICU admissions are also the result of Singapore's success in keeping numbers manageable, said Associate Professor Jeremy Lim, director of the Global Health Programme at the Saw Swee Hock School of Public Health at the National University of Singapore.
"We should appreciate that our low death rates are also because the system was not overwhelmed like in Wuhan (China) or Lombardy (Italy) which had death rates much higher than in other parts of China and Italy respectively," he said.
"Of course, beyond having a manageable number of patients, this good fortune is built on decades of investment in the health system, including sending so many of our doctors and other health professionals to train in the best centres globally."
In the longer term, the pandemic has signalled the importance of maintaining investments in health and healthcare, not just in equipment and facilities but also in human capital, Prof Lim said.
At a virtual press conference on July 7, Health Minister Gan Kim Yong, who co-chairs the task force tackling the Covid-19 outbreak, also said that the vast majority of patients here over the past few months have been young and able to recover on their own, keeping the need for hospital care or critical care low.
This also contributed to Singapore's ability to keep its healthcare system from being overwhelmed.
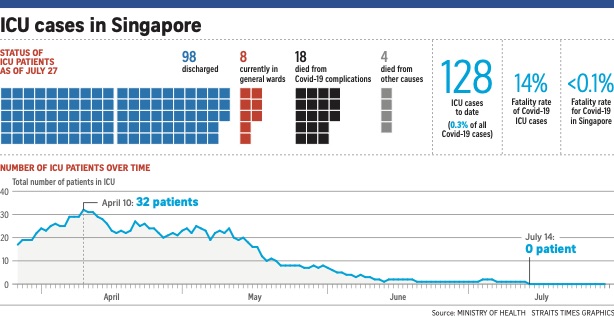
STRAITS TIMES GRAPHICS
Preparedness is another key factor, with healthcare facilities taking active steps to ensure they have enough capacity to cope with any potential surge in coronavirus cases, converting their regular wards into Covid-19-dedicated ones, and training their staff to deal with coronavirus patients.
And the community's role in keeping infection numbers low cannot be overstated, said experts.
Mr Gan said at the July 7 press conference: "We should never take for granted that our healthcare capacity is always there.
"We should always be careful and we should always do our best to minimise community transmission because from our experience, we have also seen that the increase in the number of cases can be quite exponential... Therefore, we always have to be vigilant and minimise the risk of transmission."
Other than having a robust and resilient healthcare system, preventive steps to protect citizens from Covid-19 are just as paramount, Dr Phua stressed.
A comprehensive public education system and compliance from the public when it comes to guidelines like mask wearing and safe distancing are critical in slowing the spread of the virus, Dr Phua said.
"A good public health system should not only inform people to keep to the spirit of the rules, but also have a thorough enforcement system to catch recalcitrant offenders."
Post-pandemic, an examination would be needed of how Singapore should allocate the use of its healthcare facilities, said Prof Lim.
"Do we have enough surge capacity? What should our planning parameters be? There is a cost to carrying excess capacity in peacetime and we only appreciate and thank our lucky stars we have these in times of crisis," he noted.
On the international front, Singapore should also be ready to contribute as a responsible member of the global community to capacity building in other countries that need support, and share its expertise and lessons generously, he added.
This article was first published in The Straits Times.
For the latest updates on the coronavirus, visit here.